Tesa / Tese / Pesa / Mesa

The sperm sometimes doesn’t contain the male germ cells. It also happens that the sperm obtained from the ejaculate are far from the best quality. Since the cells in the testicle have a lower fragmentation of sperm DNA, patients with certain indications undergo a testicular biopsy, a surgical procedure to extract germ cells.
When is it required?
The procedure is indicated for azoospermia meaning the absence of sperm in the ejaculate for various reasons:
- Obstructive factors. Ir can be the disruption of the duct, in which sperm production occurs, but the process of ejaculation is difficult
- Secretory disorders are associated with production in the testicle and occur with various hormonal disorders
- Genetic factors in which there are certain mutations, genetic disorders, translocations, leading to the stop or absence of spermatogenesis. Moreover, in certain situations, even such techniques as a biopsy may not give positive results. However, genetic causes are extremely rare: only 3-5% of common cases of azoospermia
What is the preparation process?
It is important to understand that you need to prepare for any surgical intervention. First of all, general laboratory tests are taken. Also, before the biopsy, non-specific or specific stimulation of spermatogenesis is performed to maximize the chances of obtaining good quality biomaterial.
In modern medicine, several methods of manipulation are distinguished. Let’s consider them in more detail.
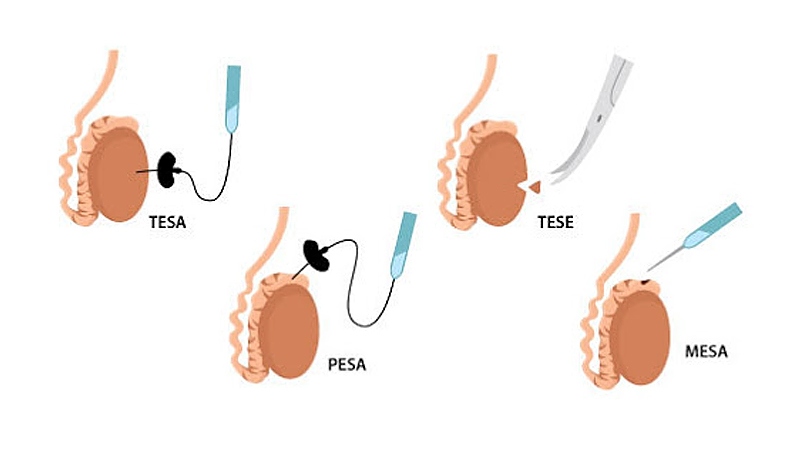
Puncture biopsy
The most popular are the PESA and TESA procedures. Puncture methods are indicated for obstructive azoospermia, when the doctor is sure that sperm can be obtained from organ tissues. These are less traumatic types of manipulation, involving the implementation of a puncture and sampling of a biopsy sample, which is immediately transferred to embryologists for evaluation. During the TESA procedure, a testicular puncture is performed, and in the PESA procedure, the puncture of epididymis is conducted.
Open biopsy
TESE and MESA are open-type procedures involving a surgical incision and obtaining spermatozoa from tissues. The seminiferous tubules are likewise transferred to the embryologist for examination, who will identify the germ cells and use them for fertilization.
Micro-TESE is considered to be one of the advanced methods. It requires the use of certain equipment – a microscope. It is usually performed in the presence of severe forms of impaired spermatogenesis, when the chances of obtaining high-quality biomaterial are minimal. As part of the operation, a small incision in the testis is made and the search for the most favorable single areas of spermatogenesis is carried out, where the likelihood of the presence of sperm cells is maximum.
Where is it carried out?
Any biopsy method must be carried out in IVF clinics or in medical centers where there is an embryological laboratory. It’s caused due to the fact that diagnostic biopsy is categorically contraindicated. Obtained biomaterial should be immediately used either for IVF / ICSI fertilization or for cryopreservation. If a biopsy is performed in a health center or a regular hospital, this can lead to a number of risks and complications, after which sperm cells may not be obtained at all.
Postoperative period
The recovery period after a testicular biopsy is not difficult. The patient is observed in the clinic for several hours, after which he goes home with recommendations from a doctor and prescriptions of drugs.
There are some medical recommendations:
- Wear underwear made of natural fabrics, put on a special bandage
- Carry out processing of the operation zone, to provide protection from the external environment
- Do not take a shower for 2 days after manipulation
On the second day after the intervention, the patient undergoes a control ultrasound. After 1-2 days, you can safely start work and continue to lead your usual lifestyle, if this is not associated with heavy physical activity.
Due to the fact that sperm cells obtained from testicular tissue do not tolerate conservation well, when a spouse has severe secretory azoospermia, it is recommended to fertilize the egg with freshly obtained biomaterial to increase the chances of success.
What are the complications after a biopsy?
Among the consequences of this procedure are distinguished:
- Swelling and pain in the operation area
- Bleeding in the operation area
- The formation of hematomas
- Inflammation
If the biopsy was performed in a good clinic by an experienced doctor, the complications after such an intervention are unlikely. If you feel unwell, you urgently need to visit a doctor and undergo a course of treatment.
Testicular biopsy is a simple operation, but its success directly depends on the experience and professionalism of the doctor. A competent doctor specializing in infertility problems knows in advance which biopsy method is best to carry out in a particular case in order to obtain the maximum result.
VittoriaVita is an international medical center with the necessary modern equipment and an embryological laboratory to conduct such research. All procedures and manipulations are carried out by reputable doctors as quickly as possible, and the presence of special cameras allows you to keep the obtained material frozen for a long time.

