What does IVF mean: details of the process
In vitro fertilization is the technology of effective assisted reproductive medicine, which is used to treat infertility. IVF gives you the opportunity to become parents in cases where alternative methods have not helped.
What is the essence of the method?
IVF is not a separate procedure, but a whole complex of procedures that can last several months. The essence of the technology lies in the fertilization of the egg outside the woman’s body. The embryo obtained in this way is transferred to the uterus for the further development of pregnancy.
Indications and contraindications for IVF
The process of artificial fertilization are practiced for various types of infertility, which could not be cured by alternative methods. Indications to use IVF:
- infertility with endometriosis
- immunological form of infertility
- male factor (poor quality of sperm)
- pathological changes in the uterine tubes or absence of organs
- mixed infertility
Contraindications to the use of the technique are diseases in the patient that interfere with the normal process of pregnancy and constitute a threat to the health of the woman and child. Contraindications for IVF:
- inflammatory processes at the acute stage of any localization
- diseases of the reproductive organs, in which the implantation of the embryo and pregnancy is impossible
- any pathological states in which child-bearing is contraindicated
- neoplasms of any etiology in the ovaries and uterus
Preparation for the process
Preparation involves a detailed examination of couples, which is necessary to:
1
identify possible contraindications for IVF
2
individually develop a hormonal stimulation timeline for a woman
3
determine the necessity for additional procedures
There is an obligate and additional list of testing.
All couples pass obligate diagnostics and additional tests are put on individually. The timeline of the upstream process is 2-3 weeks.
If after a complete examination it turns out that the ovarian reserve is depleted or completely absent, doctors offer an alternative option – the use of donor oocytes.
IVF technology in steps:treatment overview
The use of IVF is justified in the case when fertilization is impossible in a natural way. The technology is conducted on an outpatient basis in several steps.
 | Step 1. Stimulation of ovulation |
To increase the chances of success, it is necessary to obtain several mature eggs. In a woman’s body, only one matures in one cycle, therefore, superovulation is stimulated. It is develop individual timeline of hormonal therapy for women (pills or injections). This is called the “stimulation act.” The patient’s age, the reason of infertility, the state of health, and the ovarian reserve are taken into account. In the process of stimulation, follicle growth is controlled by ultrasound investigation. This allows you to correct the dosage and medications intake time. As a result of such stimulation and with good ovarian reserve, it is possible to obtain up to 10 oocytes capable to fertilization.
 | Step 2. Extraction of oocytes – puncture of follicles |
When the follicles reach the needed size, they release eggs. For this, women are prescribed hormonal medicines that stimulates the separation of mature eggs from the follicles. After 34-35 hours, the egg cells are removed from the woman’s body (follicle puncture). Selected mature oocytes that are not used in the IVF program can be frozen for future attempts, if the patients wish. This procedure is relevant for women with low ovarian reserve. If it is not impossible to take the egg from the patient there is possibility of using donor eggs.
 | Step 3. Obtaining sperm cells (sperm) |
Sperm must be obtained on the day of the extraction of eggs. The man receives the material independently by masturbation, but if it is impossible to extract sperm in this way, surgical process are used. Before the process of fertilization, sperm cells are separated from the seminal fluid, after which the best of quality of them are selected. If the patient does not have a partner she can use the donor sperm. Married couples need the written permission of the husband to use donor sperm. This rule applies if a woman is going to independently carry out the child. If a surrogate mother bears a child, donor sperm is not used.
 | Step 4. How the IVF process goes |
Before fertilization, the eggs are cleaned, their quality is checked and prepared for the process. Sperm is processed in order to isolate the highest quality spermatozoa from it. IVF is carried out in a specialized laboratory using one of two process:
Oocytes are placed in a special nutrient place, then sperm are added there. Independent fertilization takes place within 2–3 hours.
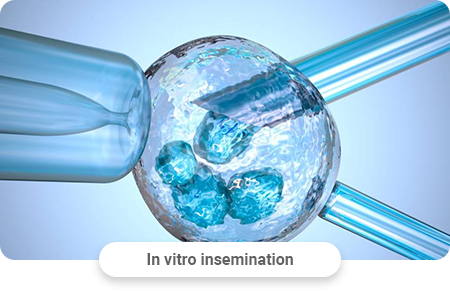
Oocytes are placed in a special nutrient place, then sperm are added there. Independent fertilization takes place within 2–3 hours.

This process is used mainly in the low quality of sperm. The highest quality sperm is injected into the egg with the help of a thin catheter. We always use the ICSI method, since it increases the chance of impregnation and pregnancy.
 | Step 5. Cultivation of the obtained embryos |
Embryos are placed in a special incubator in a nutrient medium. An embryologist monitors the development of embryos and selects the most “perspective” for transfer to the uterus. At this stage, doctors can do PGD ( preimplantation genetic diagnosis ) of embryos.
Embryos which are ready for transfer, usually froze at the blastocyst stage (5-6 days) to use for the future transfer.
 | Step 6. Embryo transfer to the uterine cavity |
Among the embryos that have been formed, several of the highest quality and suitable for the transfer to the uterus are selected. To increase the chances of implantation, we transfer two or three embryos. After this, the woman is prescribed maintenance hormone therapy, which helps the embryo to implant. After 10-14 days conduct HCG(human chorionic gonadotropin) pregnancy test. The IVF process is performed without anesthesia in most cases, since this is an useless process.. If a woman cannot bear the fetus on her own, she can use the surrogate mother services. Pregnancy does not always occur after the first attempt, some women need to undergo several procedures to get pregnant.
Pros and cons
The pros of IVF, we highlight the following:
- Solving the problem of infertility in childless couples who cannot independently conceive and give birth to a child.
- Possibility of PGD before embryo transfer.
- The ability to have a baby, even if the woman has congenital or acquired anomalies of the reproductive system.
- Ability to become pregnant at age 40+.
- Increased chances of having a healthy baby (up to 99.7%) due to a detailed diagnosis on the embryo stage
The cons of IVF:
- The probability of multiple pregnancies, since several embryos are transferred to the uterus.
- The risk of ectopic pregnancy.
- The probability of the development of unpleasant consequences while taking hormonal medicines.
- The risk of ovarian hyperstimulation syndrome (with an accurate calculation of the dose of drugs and the individual selection of a treatment timeline, the risk tends to zero).
- High cost. In case of unsuccessful attempt, it is necessary to repeat the IVF procedure, which increases financial expenses.
The above troubles can be avoided if you contact a reliable clinic. What stand attention for when choosing a clinic? On experience and number of years, qualifications of doctors, having own bank of sperm and oocyte donors in the clinic. It is necessary to take into account how many embryos are usually transferred for one act and what is the effectiveness of IVF in the clinic.
Treatment effectiveness
The success of IVF is influenced by many factors:
- patient’s age
- quality and the number of sperm cells
- number of embryos received
- properly selected program and medicines
- cause and experience of infertility
- female reproductive health
- embryo state (fresh or frozen)
- endometrial state at the time of artificial insemination
- egg state (fresh or frozen)
- qualification of doctors
Patients whose pregnancy did not occur after the IVF process should be under the care of a gynecologist.
IVF: legal situation in the USA
According to WHO statistics, the highest percentage of successful IVF program and the level of medical care remains in the United States. The US government allocates large funds for research in this area, as well as for equipping clinics of reproductive medicine.
Surrogate motherhood programs are only allowed in 8 of the 50 states. However, in 4 states this process of assisted reproductive technology is illegal.
In the United States during IVF it is allowed to choose the sex of the child. There is also the possibility of applying for insurance in case of an unsuccessful IVF program: if the pregnancy does not occur, a part of the cash is returned to the patient. The cost of an IVF program in the USA is $ 12,000- $ 20000, and an additional lawyer’s fees are paid. The final cost depends on the services that will be included in the program. For example, the choice of the child’s sex costs about $ 4,500.
The agency “VittoriaVita” offers IVF programs from 5500 to 11000 €, has the most extensive donor base in Ukraine which is constantly updates. The married couple also have a possibility to select the sex of child and PGD .
Each candidate, before becoming a donor, undergoes a detailed medical examination.
These arguments are enough to select VittoriaVita among other clinics for participation in the IVF program. You can receive the full information about programs of treatment of infertility from our managers at personal consultation.